What is a D-Dimer Test? "We avoided an emergency last week."
Last week was an intense 5 days. The D-Dimer Test was simple and key to avoiding an emergency hospitalisation.
Hello! If you’re new to Carer Mentor, welcome! Thank you for being here!
I’m Victoria, and you can read why I’m publishing Carer Mentor here: Who Started Carer Mentor and Why?
The Carer Mentor website is a hub of tools, resources & insights, as well as a community support network. A portal of hope ❤️ Start exploring here.
Dear Friends,
Last week, Monday to Friday, was an intense 5 days, but we avoided a crisis hospitalisation. So I’m feeling deep gratitude for our doctors, relief and very tired.
Know when to ask whether a D-Dimer test is appropriate for you and your loved one.
Recommendation: Learn about the D-Dimer test
More resources
Medline: What is a D-Dimer Test
“A D-dimer test looks for D-dimer in blood. D-dimer is a protein fragment (small piece) that’s made when a blood clot dissolves in your body. D-dimer isn’t usually found in your blood unless your body is making or breaking up blood clots.”
VeryWell Health What Is the D-Dimer Test? By Richard N. Fogoros, MD
“A D-dimer screening test may be used if a healthcare provider is concerned about deep vein thrombosis (DVTs)1, pulmonary embolism (PE) in the lung, stroke, or other conditions linked to blood clots.”
Mayo Clinic Symptoms, When to consult a doctor, Causes, Risk Factors
How does COVID-19 affect the blood? (includes video explanation)
“Some people with COVID-19 develop abnormal blood clots, including in the smallest blood vessels. The clots may also form in multiple places in the body, including in the lungs. This unusual clotting may cause different complications, including organ damage, heart attack and stroke.”
BUPA healthcare DVT Complications:
“A pulmonary embolism happens when a blood vessel in your lungs becomes blocked. If you have a DVT, the blood clot may dislodge or a piece may break off and travel in your bloodstream to your lungs. Here it can get stuck in a blood vessel, causing a pulmonary embolism. A pulmonary embolism can stop blood reaching your lungs properly, causing chest pain and difficulty breathing. This can be fatal if you don’t get treatment quickly.”
Background
I first discovered the D-Dimer test when my mother was hospitalised with COVID and pneumonia in 20242. There is evidence of a higher risk of blood clots and pulmonary embolism for immunocompromised patients with COVID.
I advocated for a D-Dimer test because there were no beds in the hospital respiratory ward, and there was a push to activate the ‘Virtual Ward’ system, aka I’d care for my mother at home, whilst providing the nurse team with observation readings of temperature, oxygen, BP and general health three times a day.
Virtual wards place the burden of observation and the responsibility of flagging issues on the carer’s shoulders. The time to medical intervention for an issue would be longer than in the hospital.
Imagine the emotional angst and stress on carers and mix in being informally recruited to meet the reporting needs of a nurse team, and their schedule.
So, at the time, (whilst suffering COVID and pneumonia myself camped out in the hospital), I insisted on the D-Dimer test to ensure my mother had no risk of DVTs or PEs at home.
A new equation I’ve learnt this week:
One very big swollen leg, that becomes worse over 2 days, requires urgent investigation and treatment for possible Deep vein thrombosis (DVT).
There are several high-risk factors when that leg belongs to an 80+year-old with less mobility, who’s receiving hormone drug therapy for one of her cancers and a drug treatment that affects epithelial cells for another cancer.
[Please consult your doctor if you have a swollen leg, suspect a DVT or dial emergency services if you also have chest pains or breathlessness. This article is for awareness purposes only. I’m not a doctor and cannot offer medical advice.]
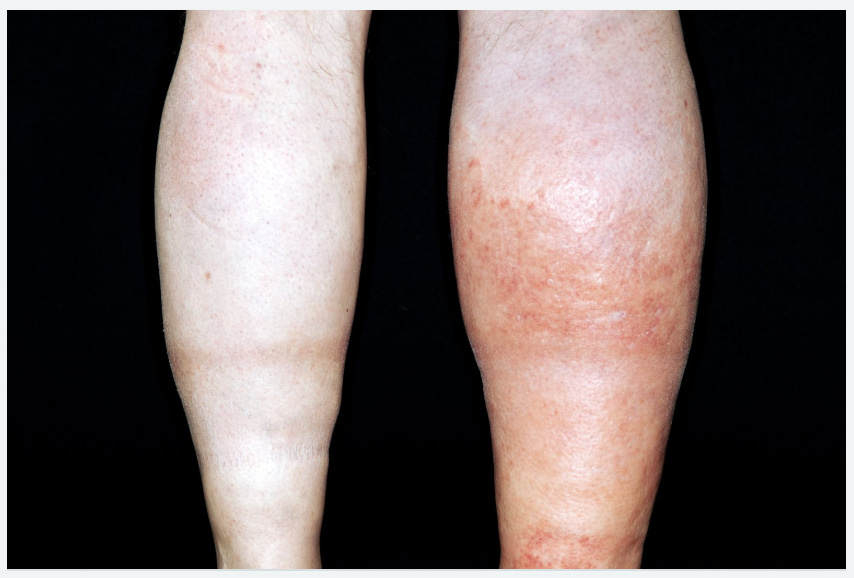
I’m very grateful
to our oncologist, who received my email with photos for our usual consultation and immediately elevated the urgency about a possible DVT. Either he could ask for an ultrasound-Doppler scan, or I could alert our GP. We decided on the latter.
to our GP practice for their triage system, and rapid response that activated the blood test and ultrasound scan
I’m glad I knew to ask if a D-Dimer test could be done, so the GP and I could agree on a plan of action together if it were positive.
Our plan of action and goals with the GP practice
Get blood taken as soon as possible, for the test to be done, and if positive, the GP would make a prescription for an anticoagulant. The goal was to have the blood thinner prescription before the weekend, if required.
An urgent request for an ultrasound Doppler scan was made at the same time, to confirm the diagnosis, but it could take 2-3 days. This is why the GP used the D-Dimer test as the trigger for the prescription, not the ultrasound diagnostic test.
Communication: I made sure to highlight the timeline of symptom worsening, current drug treatment, the cancer, the last consultation, and the oncologist’s recommendation for action.
This Carer’s accounting of actions (over 5 days). ‘Red flag’ actions on top of ‘usual’ medical appointments
I’ve counted all the actions, tests, appointments, and telephone calls over the last 5 days, in addition to the already scheduled medical appointments.
2 sets of blood were taken (Monday and Thursday morning), the second was for an urgent D-Dimer test.
3 hospital appointments: 2 pre-scheduled. We were called on Friday, late morning, for the ultrasound scan at 4.30 pm. We’re SO grateful to be squeezed in.
4 Dr telephone consultations: 1 scheduled. 3 responding to the issue: 1 to discuss and make an action plan, and 2 about test results and next steps.
2 updates to our 2 sets of oncologists
1 rapid prescription picked up.
Confirmed the anticoagulant medication instructions for use and made sure my mother and I are clear about its administration.
I re-primed us for an emergency: 1-pager Medical summary was updated with results, and Hospital GoBags double-checked.
I don’t usually do this kind of summary or dwell on these numbers, especially because they blur into what I consider my agility as a carer.
Rumination is not helpful, so I’m not laying out the detailed sequence of events. It also wouldn’t add any value to you, as these circumstances are unique to us.
I did this “accounting of actions’ on Friday as part of my journaling because I wondered why I was pushed to my absolute limit on Thursday. It felt uncharacteristically extra tough.
What pushed me wasn’t the caregiving events, but the additional ‘official’ meetings I’d scheduled for my business. Twice during the day, my flashlight of attention had to be shifted away from my caregiving priority. The constant switching of attention can easily amplify stress and strain.
Engaging in scheduled business meetings that required more administrative work and responses between medical actions was frustrating. But that’s what happens when things collide.
My adrenaline was higher than usual while monitoring for worsening symptoms and being primed for an emergency. You may know what happens if a blood clot travels to different parts of the body. My father had a couple of mini strokes/ transient ischaemic attacks (TIAs) because of blood clots. I was worried about a pulmonary embolism for my mother.
Bottom line, the blood thinner treatment has started, and I’m SO relieved we’re not in limbo over the weekend. We’re having a quiet weekend now.
Caregiving gears are ratcheting down. Completing the ‘stress cycle’ is important - so I journaled, texted friends, and walked 4km
This article is part of my re-centring because I need to know more people are aware of the D-Dimer test, especially as we’re approaching high-COVID season.
I hope this helps you.
Take care of yourself and each other. xo
Please like ‘❤️’ the article to guide others here.
If you know someone who could benefit from these resources, please share Carer Mentor with them. Please share this article/restack in Substack so others can find these resources. Thank you!
If you found this article useful, please consider upgrading to paid subscription
Deep Vein Thrombosis (from the NHS website)
DVT (deep vein thrombosis) is a blood clot in a vein, usually in the leg. DVT can be dangerous. Get medical help as soon as possible if you think you have DVT.
Symptoms of DVT (deep vein thrombosis)
Symptoms of DVT (deep vein thrombosis) in the leg are:
throbbing pain in 1 leg (rarely both legs), usually in the calf or thigh, when walking or standing up
swelling in 1 leg (rarely both legs)
warm skin around the painful area
red or darkened skin around the painful area – this may be harder to see on brown or black skin
swollen veins that are hard or sore when you touch them
ALERT: Be Aware. This is COVID Autumn 2024. UK Carers prepare yourselves! An article I wrote sharing my learnings about advocating and caring for my mother through a hospitalisation with COVID and pneumonia.


Thank you, Victoria. I had never heard of this. Great job being proactive, and advocating for your mom to get what she needed. It also shows the importance of having a good relationship with your loved one’s doctors. And about the exhaustion… the is probably the biggest contributor to my caregiver exhaustion right now—the whiplash of constantly, quickly switching between various responsibilities and roles.
So sorry you and your mum had a tough week, Victoria. I would hope - am sure - the DDimer test would have been suggested without you having to ask for it with the symptoms and risk factors your mum presented with.
One thing to watch for is the doppler ultrasound is a yes/no and the DVT service will manage it if it’s a yes ( clot ) but if it’s a no ( no clot ) that’s great, but they will then advise you to go back to the GP, to work out what it is, the most common things being cellulitis ( infection needing antibiotics ); venous insufficiency which can benefit from support stockings; calf muscle injury; or a ruptured bakers cyst ( back of knee, related to osteoarthritis and gravity takes the fluid from it down into the calf ).
I hope the weeken brings you some rest from the appointments. ( Why do these things always happen on a Friday! ? )
Oh snd I’m totally with you on virtual wards. Happened to us once, with the additional joy of them saying, but bo nurse visits cos you’re a doc, you can do it. Which meant I basically managed him myself. xx